The Delta variant is posing new challenges for Australia, as for many other countries in the world.
Previously known as B.1.617.2, the variant was first discovered in India in February, where it led to an exponential wave of infections.
According to GISAID, a data-sharing initiative for corona and influenza virus sequences, the mutation has been detected in 78 countries, and is prevalent in Britain, India and Russia.
With lockdowns currently underway in parts of Australia, we asked Sanjaya Senanayake, Infectious Diseases Physician at Canberra Hospital and Associate Professor at The Australian National University Medical School to explain how this variant spreads and to bring clarity around vaccine safety and effectiveness.

How can the Delta variant spread, and how long do people need to be in contact for it to spread?
Professor Senanayake: The Delta variant is still the same SARS-CoV-2 virus that has been causing COVID-19 since the start of the outbreak. It is just a more infectious version.
The US Centers for Disease Control and Prevention (CDC) notes that the virus spreads in three main ways:
Breathing in air with very small fine droplets and aerosol particles that contain the infectious virus. The risk is greatest within 1-2 metres of an infectious person where the concentration of the infected particles is greatest. This is more likely in enclosed places with poor ventilation.
Exhaled droplets and particles falling onto your nose, mouth or eyes when an infected person coughs or sneezes (i.e., “splashes and sprays”, such as being coughed on).
Touching your mouth, nose or eyes with dirty hands that have viral particles on them, for example, by touching a contaminated surface.
In terms of how long people need to be in contact with an infected person, the following applies, as explained by the Australian Department of Health:
- "had face-to-face contact for any amount of time or shared a closed space for at least 1 hour with an infected person during their infectious period
- "been to a venue or location where the risk of transmission is considered high e.g. a super-spreading event.
The Delta variant is more infectious than earlier variants of the virus.
For example, two people with the original Wuhan strain could infect five other people; but, two people with the Delta variant can infect 10 people.
In other words, it is twice as infectious. We have also seen some instances where people with the Delta variant may have passed to another person with a really brief or "fleeting" contact.
How can people prevent the Delta variant from spreading?
Professor Senanayake: There are lots of ways in which you can make a difference.
1. If you have symptoms that could be COVID-19, no matter how mild, please get tested and isolate at home till you have a negative result. It appears that the Delta variant causes milder symptoms than earlier strains; therefore, something as simple as a runny nose, sore throat or headache could be the Delta variant. Of course, fevers, cough and the other symptoms of COVID-19 can occur as well.
2. Use the QR code app whenever you enter a venue. This will make it so much easier for contact tracers to find you if you are part of an outbreak, and make it less likely that you could spread COVID-19 to others.
3. Avoid large gatherings where possible.
4. Follow the health advice in your area about mask-wearing.
5. Practise physical distancing where possible.
6. Wash your hands with soap and water, especially after eating or going to the toilet. Use hand sanitiser if soap and water aren't available.
7. Get vaccinated against COVID-19.
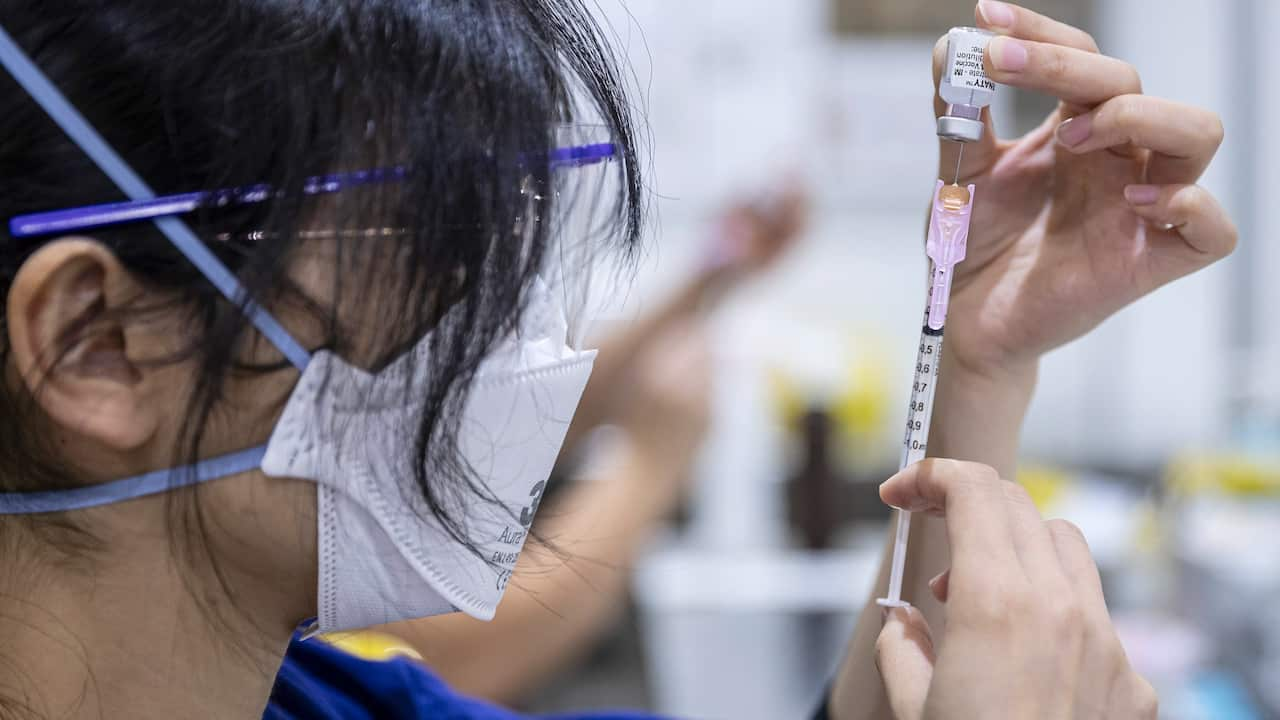
COVID-19 - Impacts on health
Can also young and healthy people get very sick from COVID-19?
Professor Senanayake: Yes, young and healthy people can get very sick, and even die from COVID-19.
In the current NSW outbreak of COVID, it is known that a number of young people (including one teenager) were admitted to Intensive Care Units because they were so sick with COVID-19.
US data looked at 601,124 deaths from COVID-19. They found that 28,354 deaths (4.75) occurred in people aged between 18-49 years old. So while it is not common, young people can die from COVID-19."
What’s the chance of a young and healthy person ending up in hospital with COVID-19, and in ICU?
Professor Senanayake: People in the US aged between 20-54 years old made up 38 per cent of hospitalisations in a series of cases of COVID-19.
According to CDC data, in severe cases, people aged from 20-44 years old made up 12 per cent (1 in 8) of Intensive Care Unit (ICU) admissions with COVID-19."
Are there percentages available that outline the risk of ending up in hospital with COVID-19 for the different age groups?
ProfessorSenanayake: This table on the US CDC website looks at hospitalisation and death risk relative to 18-29-year-olds.
Can COVID-19 leave long-lasting damage in a person’s body?
Professor Senanayake: Although it seems like COVID-19 has been with us for ages, it has only been one-and-a-half years. So we are still learning about the long-term effects of COVID-19.
But there is a phenomenon called 'Long COVID' or 'Post-acute COVID-19 Syndrome'.
This can be associated with a variety of mental and physical symptoms such as headache, joint pains, muscle weakness palpitations, anxiety/depression. In some people, these symptoms persist months after having the acute episode of COVID-19.
An examination of almost two million US insurance claims showed that you don't have to be sick with your acute episode of COVID-19 to have "Long COVID" symptoms.
Even 19 per cent of people who had no symptoms (asymptomatic infection) and 27 per cent of those with only a mild-moderate COVID-19 acute illness went on to have chronic symptoms."

Vaccines - Side effects
There has been a link between the AstraZeneca vaccine and a rare condition called thrombosis with thrombocytopenia syndrome (TTS). What is it and what are the chances of developing these side effects?
Professor Senanayake: Currently, according to the Australian Technical Advisory Group on Immunisation (ATAGI) the risk is:
- 2.6 per 100,000 in those <60 years; and
- 1.7 per 100,000 in those ≥60 years.
- 1 in 1,200,000 risk of dying (5 deaths from 6.1 million first doses of the AstraZeneca vaccine).
There have been rare reports of heart inflammation (myocarditis) or inflammation of the heart membrane (pericarditis) after the second dose of Pfizer. What are the chances of developing these side effects?
Professor Senanayake: It is suspected that the Pfizer vaccine can be associated with this side effect.
It appears to be rare with just over 1000 cases reported in the US in the context of over 177 million people having received at least one dose of vaccine. It has usually been seen in male adolescents and young adults aged 16 and over. Cases are usually temporary and get better by resting. Some people need to be hospitalised.
It is very important to remember that COVID-19 is more likely to cause myocarditis and pericarditis compared to the Pfizer vaccine.
Do the benefits of the AstraZeneca and Pfizer vaccine outweigh the risk of serious illness or death from COVID-19? Are there any statistics available?
Professor Senanayake: ATAGI is the vaccine expert group advising the government. They have said that for all Australians 60 years or over, the benefits of vaccination with COVID-19 Vaccine AstraZeneca strongly outweigh the risks. ATAGI looked at three scenarios where there are different rates of COVID-19 in the community.
They concluded that the benefits of getting the AstraZeneca vaccine to prevent severe COVID-19 outweigh any risks for ALL adults (not just older adults) in medium and high-risk exposure situations.
In other words, during a COVID-19 outbreak where there's limited access to the Comirnaty (Pfizer) vaccine, ATAGI reinforces that adults younger than 60 years old need to re-assess the benefits of being vaccinated with COVID-19 Vaccine AstraZeneca, versus the rare risk of a serious side effect. This would mean having a talk with your local doctor."
What are normal and temporary side-effects from these two vaccines?
Professor Senanayake: As shown in the latest COVID-19 vaccine weekly safety report published by the Therapeutic Goods Administration (TGA), the most common side effects reported from these vaccines are mild and expected. These are headache, muscle pain, fever, chills and injection site reactions.
Are these two vaccines safe for pregnant women?
Professor Senanayake: Currently in Australia, as per advice from the TGA, the Pfizer vaccine is recommended for pregnant women. In pregnancy, there is a higher risk of a severe COVID-19 illness and a higher risk of a premature birth.
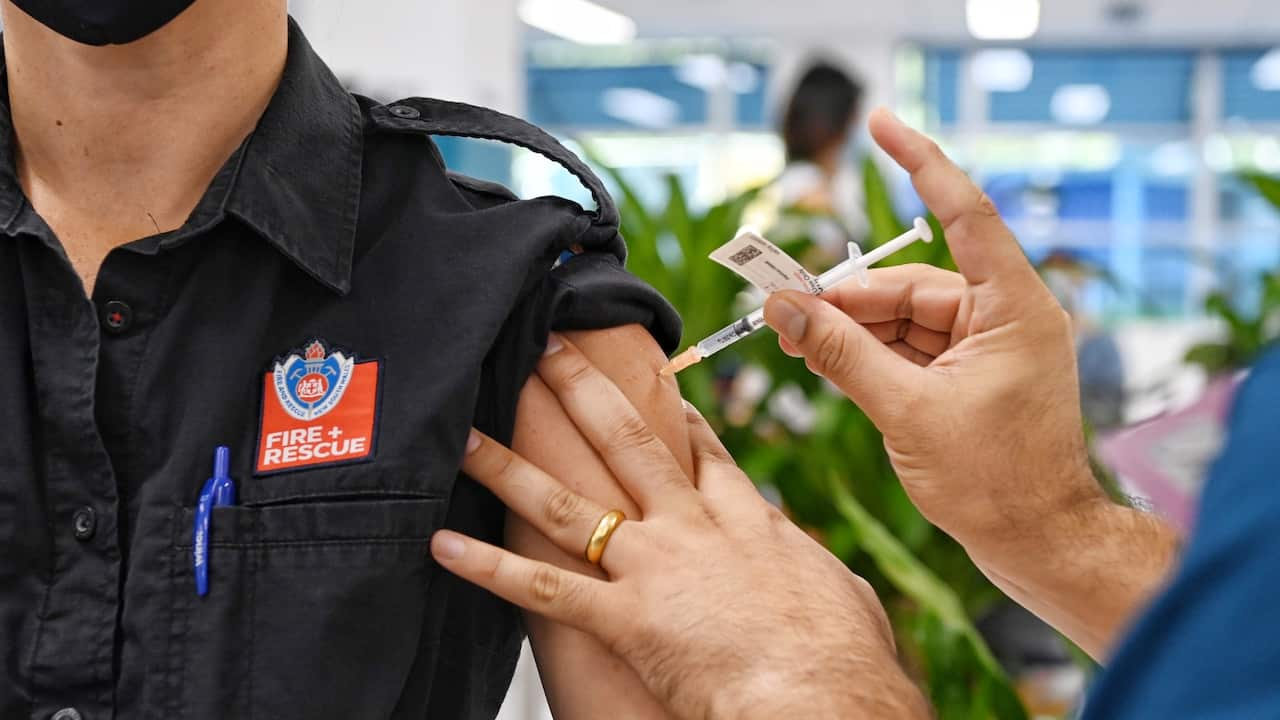
Vaccines — Effectiveness
What are the rates of effectiveness against symptomatic infection by Delta variant for the AstraZeneca and Pfizer vaccine after the first and the second dose?
Professor Senanayake: Data from the UK has shown that two doses of the AstraZeneca vaccine and two doses of the Pfizer vaccine were 74.5 percent and 88 percent effective at preventing symptomatic infection with COVID-19. This is good.
Importantly, one dose of either vaccine was only 30.7 percent effective. In other words, it is vital to get both doses of either vaccine. One dose isn't very useful."
How effective are the AstraZeneca and Pfizer vaccines in preventing hospitalisation with the Delta variant?
Professor Senanayake: UK data showed that two doses of either vaccine provided more than 90 percent protection from hospitalisation with COVID-19. This is a really important statistic and demonstrates the benefits with getting fully immunized with either the AstraZeneca or Pfizer vaccines.
Quarantine, travel, testing clinics and pandemic disaster payment
Quarantine and testing requirements are managed and enforced by state and territory governments:
NSW Travel & transport and Quarantine
VIC Travel permit, Overseas travellers and Quarantine
ACT Transport and Quarantine
NT Travel and Quarantine
QLD Travel and Quarantine
SA Travel and Quarantine
TAS Travel and Quarantine
WA Travel and Quarantine
If you want to travel overseas, you may be able to apply online for an exemption. Click here for more information about the conditions to leave Australia. There are temporary measures for international flights that are regularly reviewed by the government and updated on the Smart Traveller website.
- News and information over 60 languages at sbs.com.au/coronavirus
- Relevant guidelines for your state or territory: NSW, Victoria, Queensland, Western Australia, South Australia, Northern Territory, ACT, Tasmania.
- Information about the COVID-19 vaccine in your language.
Visit the NSW Multicultural Health Communication Service's translated:
COVID-19 Vaccination Glossary
Appointment Reminder Tool.
Testing clinics in each state and territory:
Pandemic disaster payment information in each state and territory:
