In brief
- Australia recorded its deadliest flu season this century in 2025, with more than 1,700 deaths.
- Experts are concerned about declining vaccination rates, with some Australians underestimating the risk of influenza.
Australia has recorded about half as many influenza cases this year compared with the same time last year, but experts warn the threat is still not being taken seriously enough after the deadliest flu season this century.
Nearly half a million influenza cases were reported to the national notifiable disease surveillance system (NNDSS) in 2025 — the highest figure since NNDSS records began in 1991. Of those, more than 1,700 died, marking the deadliest flu season this century.
At a national online briefing on Tuesday, experts said this year's flu season remained unpredictable, but vaccinations were the best way to prevent serious illness.
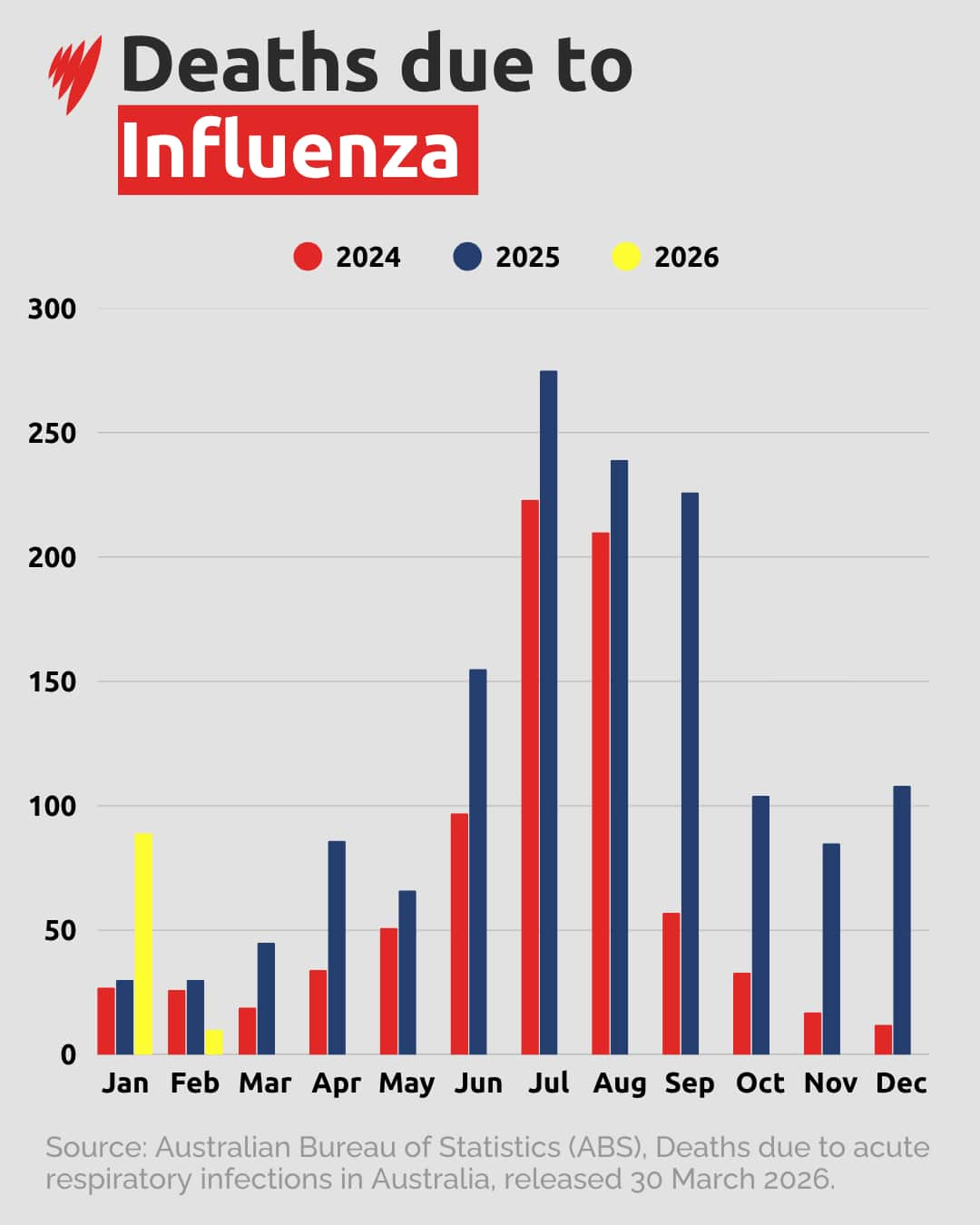
Dr Masha Somi, acting deputy director of the Australian Centre for Disease Control, said 29,300 influenza cases had been recorded so far in 2026 — about half the number at the same point last year.
Influenza activity was "currently low and relatively stable", she said, with most cases among children under nine and adults aged over 75. However, infections are expected to rise heading into winter.
In August 2025, influenza fatalities surpassed COVID-19 deaths for the first time since 2020, becoming the leading cause of death among acute respiratory infections.
Somi said last year's high fatality figure was linked to the higher number of cases, rather than a more severe strain.
More than 31,000 COVID-19 cases have been recorded so far this year, also about half the figure for the same period in 2025.
Respiratory syncytial virus (RSV) cases have also fallen 16 per cent compared with this time last year, despite a spike in February and March. Somi said the addition of the RSV vaccine to the national immunisation program likely contributed to the decrease.
She noted NNDSS figures only reflect reported cases and do not capture people who did not test or only used rapid antigen tests.
Somi said seasonal patterns vary significantly, making it difficult to predict each flu season.
"This is because some influenza viruses spread more easily than others, and some cause more severe illness than others."
Professor Patrick Reading from the Doherty Institute said last year’s season was unusual, extending into spring and marked by the emergence of a different strain, H3N2 sub-clade K, or "Super-K flu".
"In June, July and August, we (had) this peak of H1N1, influenza activity," he said.
"What happened from September and October onwards is we saw an emergence and a dominance of a different sub-type, and this was quite unusual."
He said Super-K flu became the dominant strain during the northern hemisphere winter, and while influenza activity remained low in Australia, it was expected to rise.
"We cannot predict the severity or which virus or viruses will predominate in the upcoming influenza season. We kind of have to wait and watch," he said.
He said vaccination remains the most effective protection against severe illness, and this season's vaccines would be a "better match" if Super-K becomes the dominant strain.
Professor Kristine Macartney, director of the Australian National Centre for Immunisation Research and Surveillance, warned vaccination rates were slipping and many Australians underestimated the risks.
Only 60 per cent of adults aged over 65 and a quarter of children aged between six months and five years were vaccinated for influenza last year, she said.
"Influenza can cause serious illness, it can result in hospitalisation, it can result in death. This can happen in perfectly healthy people of all ages," she said.
"The most at-risk groups are older people, infants, young children and Aboriginal and Torres Strait Islander people … [and] people with chronic health conditions."
For the latest from SBS News, download our app and subscribe to our newsletter.

