When Sydney Toro was rushed to hospital sweating, feverish and struggling to breathe in the early hours of the morning, his family feared the worst.
The 49-year-old from Cranebrook in Greater Western Sydney was diagnosed with kidney failure last year and has since had to spend five hours a day, three days a week, on a dialysis machine in hospital.
But for people like him, the coronavirus pandemic has become another threat to survival.
When Sydney was admitted to hospital with COVID-19 symptoms in April, doctors suspected he had the virus, but after days of testing, the pneumonia in his right lung turned out to be unrelated.
He spent the following days being treated not too far from the wards where COVID-19 patients were being cared for.
News that makes sense
Your trusted source for staying up-to-date with the world around you. Get free daily news updates and analysis, straight to your inbox.
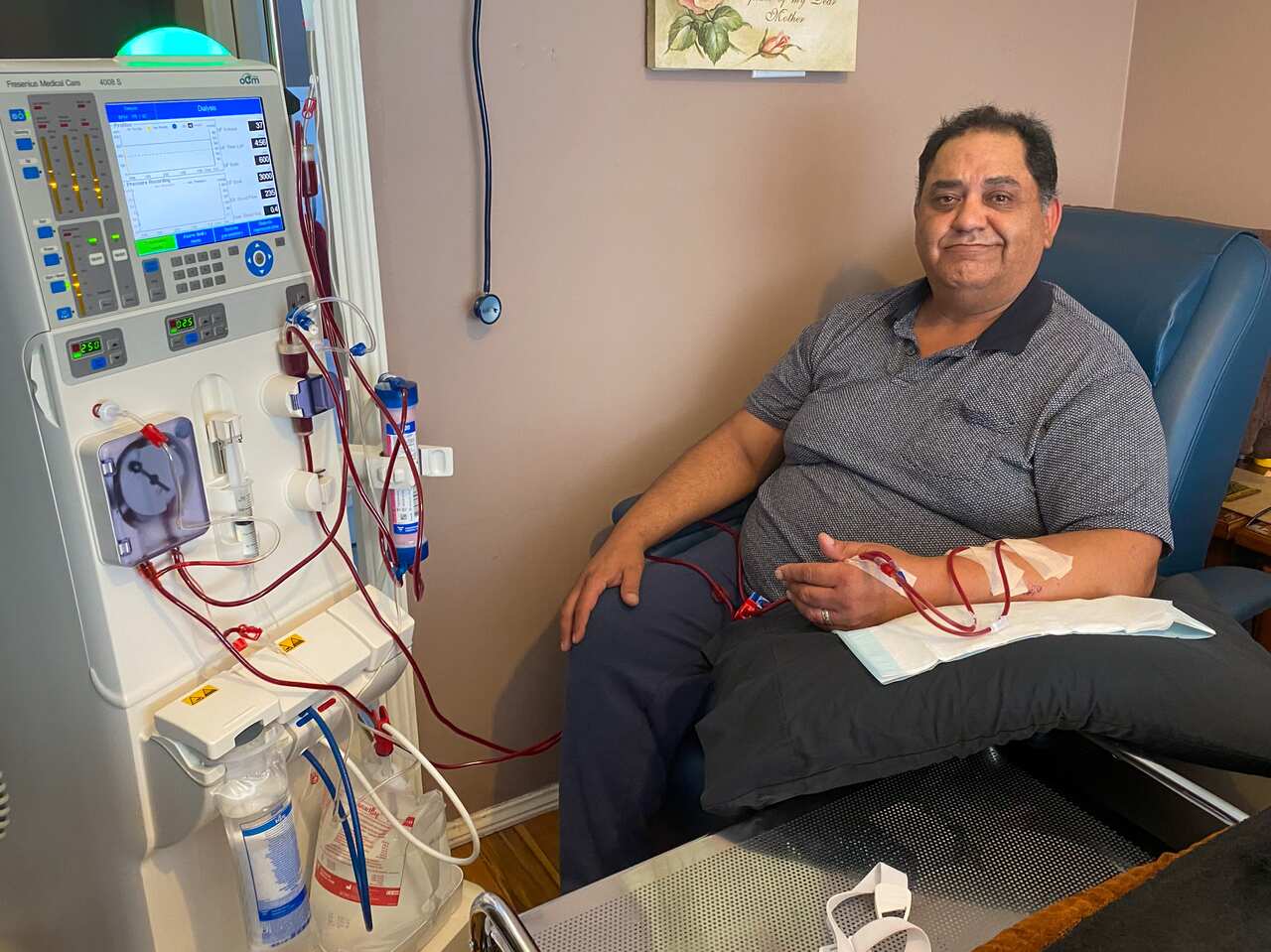
“It was daunting seeing other people around me that actually had the virus,” Sydney told SBS News. “It was somewhere I really didn’t want to be, especially in my state.”
Sydney’s doctor recommended that he and his wife Mardi instead completed a home dialysis course to avoid the risk of frequent visits to the hospital and the couple used their newly-installed machine for the first time last week.
“At first it was something we didn’t think we were going to be able to do,” Mardi said. “We were so nervous, but I just kept saying to him, 'we’ve got this, we can do this', and we had no trouble at all.”
While it’s been a big change for the household, the couple agrees the freedom of doing dialysis at home has changed their lives for the better.
But what Sydney really needs is a new kidney.
Growing waiting list
Sydney is one of 1,700 Australians on the waiting list for an organ transplant, and it's a wait the pandemic threatens to make even longer.
There has been a 20 per cent decline in organ donations and transplant procedures compared to this time last year.
Kidney transplants were suspended for six weeks from the end of March to May, and the travel and social lockdowns across the country meant there were fewer people being taken to hospitals, for example after roadside accidents.
“If the hospitals are quiet, and they were, you’re going to have less of those organ donors around,” said Professor Toby Coates, president of the Transplantation Society of Australia and New Zealand.
CEO of the Organ and Tissue Authority Lucina Barry said changing border restrictions and a reduced number of flights have also posed new challenges in getting organs to recipients.
“The organ will go to the highest match. That match may not be in your hospital or even in your state," she said.
“On one occasion we had to use a private jet to retrieve organs so the recipient didn't miss out on a transplant.”
Organs are also primarily transplanted from people who die in intensive care, a section of hospitals which would need to be reserved for the most severe COVID-19 patients.
Professor Peter Macdonald, a senior staff cardiologist in St Vincent’s Hospital’s Cardiopulmonary Transplant Unit, is concerned about what would happen if intensive care units fill up with critically ill patients with COVID-19.
“There’d be no other beds for people who might die in circumstances where organ donation is possible,” he said.
And while potential donors are screened for COVID-19, Ms Barry said: “what you don't want to do is transfer an infectious disease through a transplant recipient who then doesn't survive”.
Why donors matter
Neha Gupta was fortunate enough to receive a kidney transplant before the pandemic.
After spending 11 hours a day on a dialysis machine for five years, she was told she had a second chance at life on her 35th birthday.
While waiting for a transplant, Neha missed both her sisters’ weddings, was unable to visit her parents in India, and was too weak to spend quality time with her now 13-year-old daughter, Siya.

“I was very fragile so I missed all those moments like playing with her and teaching her how to ride a bike, and I’ll never get that time back,” she said.
Neha and her family said they are forever grateful to the person whose kidney she received.
"I would want to meet them in real life," her daughter Siya said. "I would want to pour my heart out to them and how grateful I am because it's made a person I live with happier."
After her transplant, Neha’s doctor told her that all her own organs, except her kidneys, could be used to save someone else’s life in the future too. That’s when she registered to become an organ donor.
Ms Barry said it is important to spread the word about organ donation.
“We've got a lot of Australians that don't know about it.”
“It’s important people talk to their families and if they support it, go to the national register and register that they want to be a donor."
DonateLife Week is marked this week and encourages Australians to understand organ and tissue donation and sign up to become a donor. For more information visit donatelife.gov.au.

