HIV diagnoses among heterosexuals have increased by 10 per cent over the past five years, according to new statistics.
The Kirby Institute at the University of New South Wales released the new statistics on Monday and will present them at the Australasian HIV & AIDS Conference in Sydney this week.
The research found more than half of the diagnoses among heterosexuals were late, meaning that the patient had been living with HIV for four or more years.
News that makes sense
Your trusted source for staying up-to-date with the world around you. Get free daily news updates and analysis, straight to your inbox.
“Being diagnosed late can affect a person's immune system and their health and they also might pass on infection unknowingly to someone else,” said the Kirby Institute’s Professor Rebecca Guy.
She said heterosexual males are emerging as the fastest growing group of HIV diagnoses, with a 19 per cent increase in the last five years.
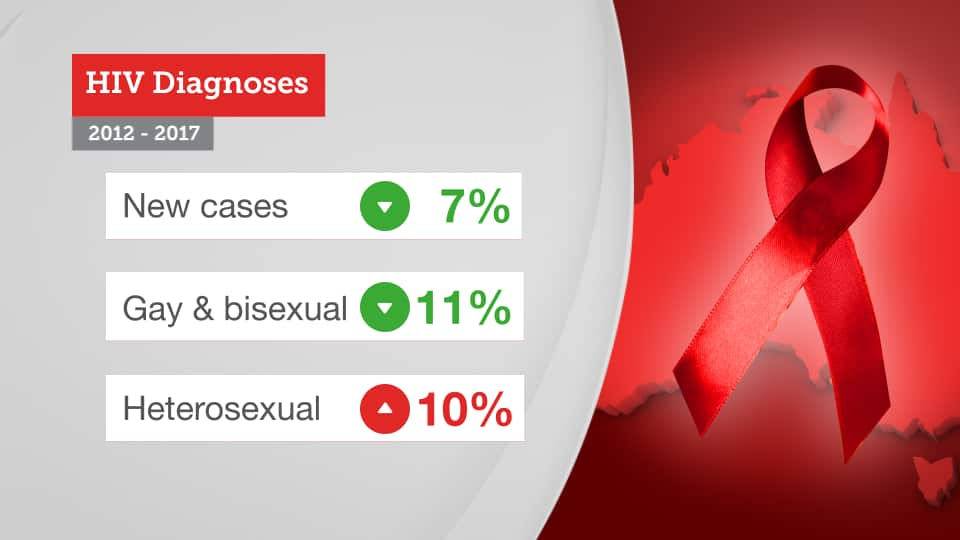
A seven-year low
The overall number of new diagnoses of HIV in Australia last year dropped to a seven-year low, dipping below 1000 to 963 new diagnoses.
That drop has been mainly attributed to a 15 per cent fall in the diagnosis of HIV among gay and bisexual men – traditionally comprising almost two-thirds of people infected with HIV in Australia.
Authorities credit the higher rates of testing and treatment, as well as an increase in the use of the preventative "prep" pill, also known as pre-exposure prophylaxis.
Prep is used before sex, similar to an oral contraceptive pill, and was listed on the Pharmaceutical Benefits Scheme in April.
But despite the progress, Professor Guy said more work needs to be done to lower the diagnosis rates in certain groups, including migrant communities.
"The declines in HIV have not been equal,” she said.
“There have been no major declines in people born overseas, and there's also been an increase in heterosexuals, which highlights the importance of additional, tailored strategies to ensure the benefits of Australia's prevention response are equitable."
In the last five years, while the number of diagnoses have dropped by 25 per cent among men who have sex with men, the numbers have increased by 5 per cent for men born overseas.
'Thriving' with HIV
Richard Keane, chief executive of support group Living Positive Victoria, understands the initial fear of getting a diagnosis of HIV.
He has been living with HIV for 27 years and said the biggest challenge he grappled with was self-stigma.
“I always prepared to possibly die from AIDS,” he said of the medical advice at the time, which said he had five years to live.
“I fell off the radar for a time, and became self-isolated.”
It was after the death of his partner to an age-related illness that he decided to take action.
“I decided I need to be brave and I needed to put my face to living with HIV, and speak about the real lived experience,” he said.
“What led me to advocacy is the peer support because there are a range of challenges around discrimination, what your legal obligations are…all sorts of issues around who do you tell, when do you tell.
“I am now sharing those experiences to become resilient.”
He said early testing is critical to receiving the treatment that will facilitate a good quality of life, adding that overcoming stigma is still a concern today.
"It made me see my best days weren't behind me, they're ahead of me, and I am living well, and I'm thriving with HIV,” Mr Keane said.
“We need to move away from the old idea that HIV is a gay disease...a lot of people in the heterosexual community don't think they're at risk.
"But if we're going to genuinely end HIV, I need to remind people that everyone is at risk of HIV. I encourage you to go to your doctor and get a HIV test."
HIV in Indigenous communities
Associate Professor James Ward, head of Aboriginal Infectious Diseases at the South Australian Health and Medical Research Institute, said Aboriginal populations in regional areas also need particular attention.
“A common theme over the last five to 10 years [has been] small outbreaks in regional and remote areas," he said.
"It puts enormous strain on health services in those settings, and enormous buy-in of expertise is often required in those settings.”
The Australian government is one of the few nations that has set a goal to virtually eliminate HIV transmission, and is due to release a new national HIV strategy soon.
While there is no cure for HIV, a virus which attacks the immune system, regular treatments can suppress the virus so that the transmission risk through bodily fluids is effectively zero.
A person living with HIV receiving treatment is expected to live a near-normal life span.
If left untreated, however, the condition could lead to serious damage of the immune system and the development of AIDS (acquired immune deficiency syndrome), where life expectancy drops significantly.
The full findings from the Kirby Institute will be presented in November.
Support groups
National Organisations
Australian Federation of AIDS Organisations (AFAO):
Phone: (02) 9557 9399
National Association for People Living with HIV Australia (NAPWHA):
Phone: (02) 8568 0300
Free call: 1800 259 666
A more extensive list of support groups, including those in each state and territory, can be found here at the Next Steps resource developed by AFAO and NAPWHA.

