New research has found taking of probiotics appeared to be "useless in many cases" and could have adverse side effects when taken after antibiotics.
Experiments conducted on people's guts found that the ability of probiotics to boost the number of good bacteria in the gut depends on the bacteria already present inside the gut.
Instead of examining faeces or stool samples, researchers in Israel have for the first time took samples from inside the guts of 25 people through the use of a tube.
Generic priobiotic strains was given to one group, and a placebo was administered to the other. Results were taken before, and for the two months following the taking of the probiotic or placebo.
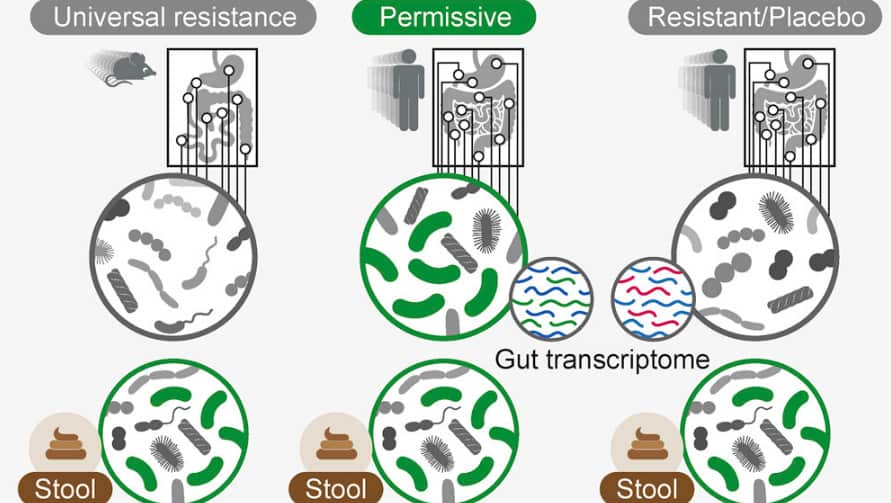
The results showed that the new samples were much more representative of how many good bacteria stay alive in a person's gut.
The authors of the research published in the journal Cell recommend that the use of probiotics be tailored to individuals based on the bacteria already in the gut, and their health needs.
"If some people resist and only some people permit them, the benefits of the standard probiotics we all take can't be as universal as we once thought," study co-author and immunologist Eran Elinav said.
"These results highlight the role of the gut microbiome in driving very specific clinical differences between people."
In a second study, conducted by the same research group, 21 people were given a course of antibiotics and then split into three groups.
The first group were given no treatment, the second group used generic probiotics, and the third was treated with a fecal microbiome transplant using their own bacteria, which had been gathered before taking the antibiotic.
The second group achieved immediate results with the antibiotics clearing the way for the probiotics to easily colonise the gut, but the process of returning the gut microbiome to a normal state took months.
"Contrary to the current dogma that probiotics are harmless and benefit everyone, these results reveal a new potential adverse side effect of probiotic use with antibiotics that might even bring long-term consequences," Elinav said.
"In contrast, replenishing the gut with one's own microbes is a personalized mother-nature-designed treatment that led to a full reversal of the antibiotics' effects."
Co-author and computational biologist Eran Segal said the study shows the universal consumption of probiotics should be tempered.
"This opens the door to diagnostics that would take us from an empiric universal consumption of probiotics, which appears useless in many cases, to one that is tailored to the individual and can be prescribed to different individuals based on their baseline features."
Probiotics can be found in supplements and fermented foods like pickles, kimchi, sauerkraut and yogurt, as well as cheese and chocolate.
A review of 313 randomised controlled trials, published in BMJ in June, found taking probiotics helped to prevent diarrhoea, bronchitis and eczema.
The studies also noted improvements in reducing heart disease risk and reducing inflammation markers in the blood.

