Jake Simpson was 22 when he started to get painful toothaches. Trips back and forth to the dentist couldn’t seem to fix the growing lump at the back of his mouth.
It came as a total surprise to Jake, his partner Carly, and their newborn son Noah, when oncologists in Brisbane told him he had stage four head and neck cancer, and would need to start treatment immediately.
“We didn’t know what any of it meant. He was so young and healthy, we couldn’t believe it,” Carly said.

Despite rigorous treatment and surgery that removed more than two-thirds of his tongue, Jake’s cancer was too aggressive and spread to his lungs.
He died within eight months of his diagnosis.
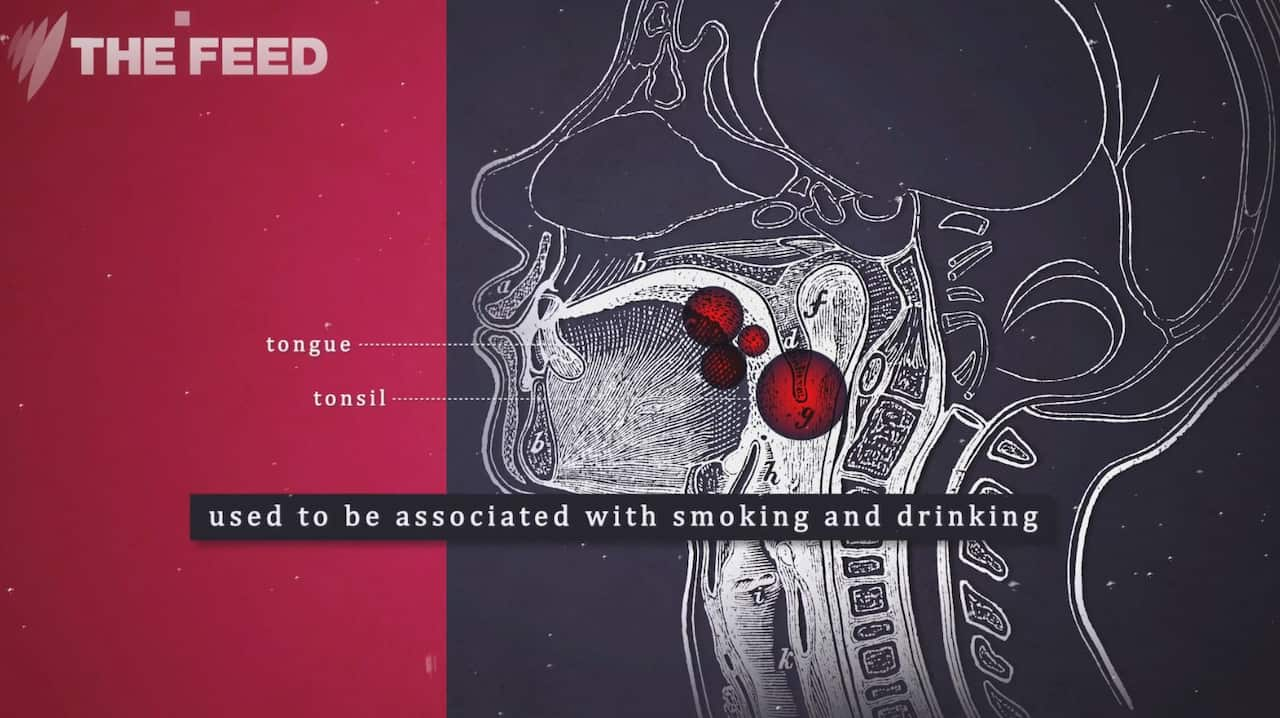
These cancers, known as oropharyngeal cancers in the back of the tongue and tonsils, are on the rise in young men, and are caused by the sexually transmitted disease HPV – human papillomavirus. While doctors believe it is most commonly passed on through oral sex, some argue it’s now as easy as ‘deep kissing’.
“Jake wasn't tested for HPV because it was too aggressive from the day one, but that age bracket that he fell in, more than likely, the cause was HPV,” Carly said.
HPV has been dubbed the ‘common cold’ of STDs. Over 80 per cent of Australian adults will get HPV at one point in their lives, and most will clear it without even knowing.
But two particular strains, P16 and P18 are closely linked with cancer, not just in the cervix like widely known, but increasingly in the head and neck.
Researchers across the US, UK and Australia say changing sexual practices over the last 50 years, and an increase in sexual partners has prompted the rising incidence rate of this cancer.
Oncologist Brett Hughes has witnessed the significant shift in the patient demographic, who says nearly 80 per cent of his patients now have HPV positive cancers.
“We now see an age group of people who generally live very healthy lifestyles; that don't necessarily have to have drunk or smoke and the other risk factors that we'd normally associate with cancers in the mouth or throat.”
The cancer is also eight times more likely to present in men.
Dr Hughes said oropharyngeal cancers are now the most common HPV related cancer in Australia, trumping cervical cancer, and are continuing to rise.
“It's predicted for Australia and it may even be as late as in the 2030s that we might see the peak incidence which is a little bit scary considering how common this cancer is becoming.”
While this cancer is increasing, many take comfort in Australia’s strong vaccination program to fight HPV related cancers.
The Gardasil vaccine, developed by Australian of the year Professor Ian Frazer, was first administered to Australian girls in 2007, and then to boys in 2013 after it became clear HPV was affecting them as well.
But Professor Frazer said people need to be given the vaccine before they’re sexually active.
“All the vaccines that we currently use are vaccines to prevent infection. A vaccine to cure an infection is a different beast all together,” he said.
Without a therapeutic vaccine, sexually active adults who missed out on the vaccine at school are still at risk of contracting persisting HPV, with Prof Frazer insisting “the big challenge now is to get something for oropharyngeal cancer.”
Right now, there is no vaccine for adults and no way of testing or preventing HPV positive oropharyngeal cancers. But there are people out there trying to change that.
After Jake Simpson passed away in 2016, he donated $20,000 for research into early intervention for these cancers.
His family chose a saliva research program currently underway at the Institute of Health and Biomedical Innovation in Brisbane lead by Professor Chamindie Punyadeera. The lab work is aimed at creating a simple and easy test everyone can do to monitor their HPV status at the dentist or GP.
“What we want to do is early intervention and detection,” she said.
“If you detect early, 80 per cent of patients survive. If you detect late, 20 per cent of them survive.”
But as the technology is still five years away from public use, and a therapeutic vaccine is perhaps even further away, Carly and Professor Punyadeera agree young people just need to be aware that this cancer exists, and is on the rise.
“Young boys think it’s a women's cancer type. It’s not at all,” Prof Punyadeera said.
“It’s really sad and we all need to be aware of HPV associated head and neck cancers.”
Through award winning storytelling, The Feed continues to break new ground with its compelling mix of current affairs, comedy, profiles and investigations. See Different. Know Better. Laugh Harder. Read more about The Feed
Have a story or comment? Contact Us


