A Western Australian grandmother said she was “at peace”, the day before ending her life under WA’s new voluntary assisted dying laws.
Mary-Ellen Passmore, 63, a Wongatha-Yamatji woman who lived with motor neurone disease for more than six years, chose to end her life with medical assistance.
She died in a Perth hospital on Thursday, one of the first people to use Western Australia’s voluntary assisted dying laws that came into effect on July 1.
“How do you describe the pain that I have endured for too long? I’m in pain constantly,” Ms Passmore said the day before she died.
“I feel very honoured to choose when and where I can die. Even if it’s in this tiny ward, I’m very happy with my decision.”
Ms Passmore’s family issued a statement, describing her as ‘a big woman in every sense – commanding, tall, vivacious, outspoken, generous, wholehearted’.
“Her life is always full of people. Her home usually had someone staying there, that needed a safe place,” the statement reads.
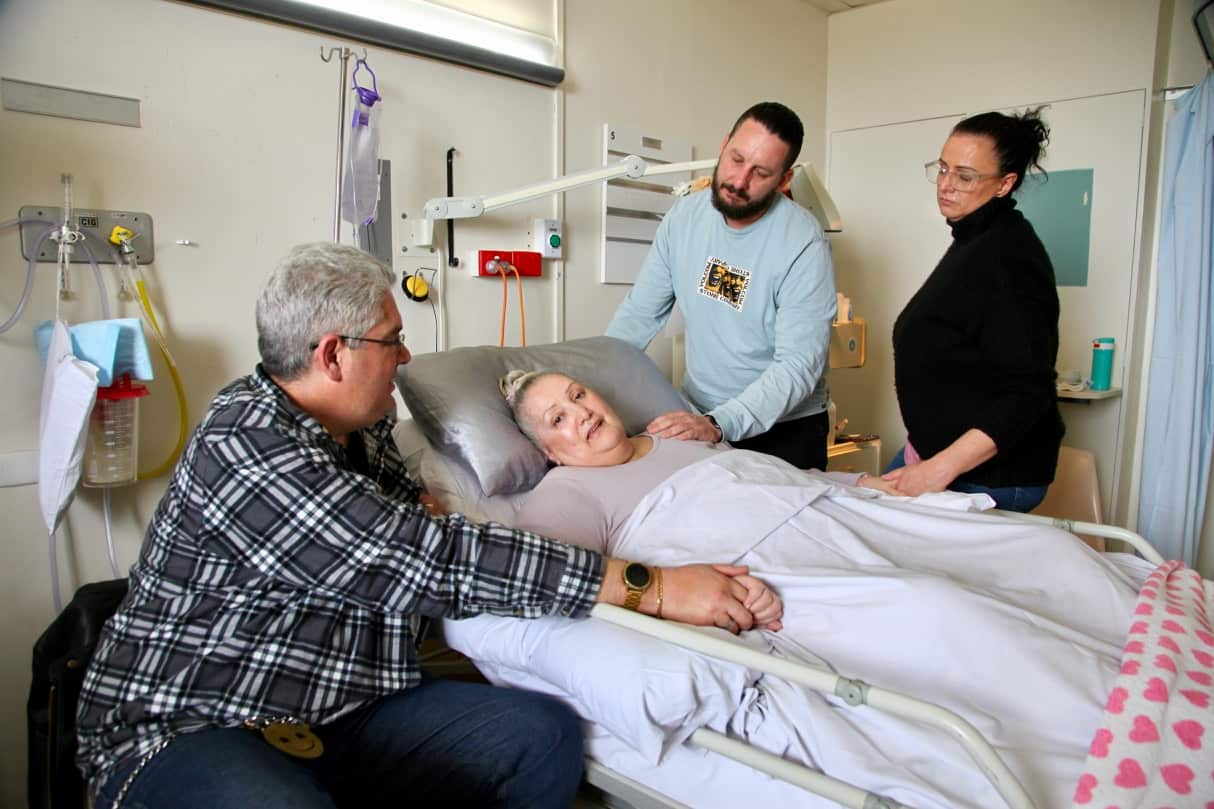
She had been admitted to hospital nine days earlier, and died surrounded by family and medical staff singing ‘Hallelujah’.
"The doctors made sure right until the end, that this is what she wanted. The care and compassion provided by the doctors made a big difference,” a family spokesperson said.
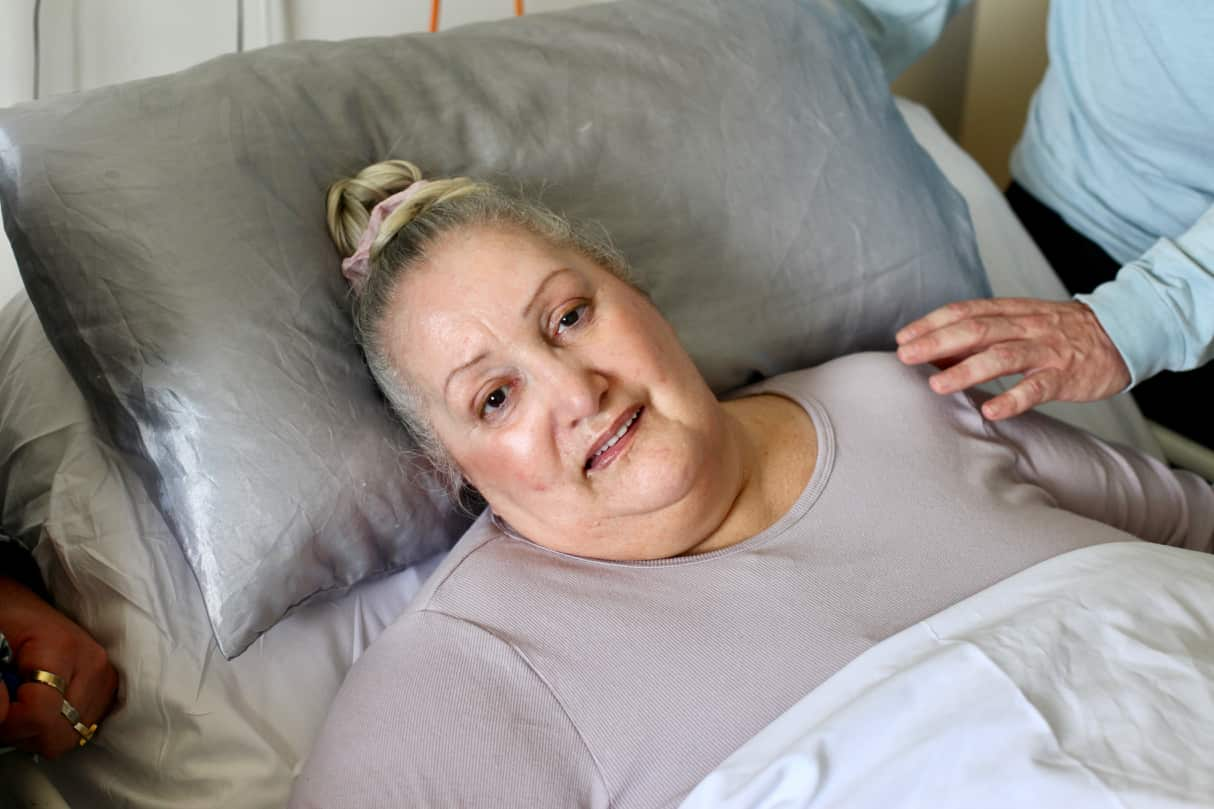
'A really strong woman'
Ms Passmore grew up the eldest of seven children in the Western Australian town of Three Springs.
She had three children of her own as well as fourteen grandchildren, and spent most of her working life developing education programs for Aboriginal communities.
“Seeing her cry in pain, (that's) not my mum," said her eldest son Challan Edwards.
She’s a strong Black woman. We’ve got a huge family and she was the leader, she was a really strong woman.”
For the past nine days, a steady stream of family and friends filed through the floor of her hospital ward, leaving vases of flowers by her bedside, and piled up on the windowsill.
“I feel at peace within myself. I have the love of my children, and they are saying, ‘yes mum, you’ve had enough," Ms Passmore said.
"And I love my children for allowing me to do this."

A worsening condition
Ms Passmore says she was first diagnosed with motor neurone disease six years ago, but had struggled with symptoms for years before.
In a person with MND, nerves that communicate between the brain and the muscles degenerate and die, causing the muscles to weaken. The condition can severely limit movement, speech and the ability to swallow and breathe.
In the early stages of the condition, Ms Passmore would injure herself falling down, but says she found it difficult to get medical help as an Aboriginal person, often dimissed by health workers as an angry Black woman.
“Those years were horrific. I kept falling over backwards, and the only thing that stopped me from getting concussion was the bun I used to wear at the back of my head to keep it nice and neat and tidy. And that saved me so many times,” she said.
Ms Passmore began using a walking frame for a period but her condition worsened. She received in home care, as well as support from MND Society.
“Nothing was too much hassle for them, from specialised wheelchairs to food,” she said.
At the time of her death, she had become totally bedridden, she had difficulty speaking and swallowing and was fed through a tube.

How the laws work
On Thursday, before Ms Passmore died, WA Premier Mark McGowan announced in a Facebook post that the first person in the state had chosen to end their life under the laws.
The laws first passed at the end of 2019 with 55 amendments, after hours of heated debate in the upper house.
Ms Passmore watched the parliamentary debate closely, after first telling her family of her desire to access assisted dying several years ago.
“The fact that it’s going to stop is a relief, it really is. (The pain) is going to be over for her. If she wasn’t suffering, I’d be against this. But the amount of suffering is unreal,” Mr Edwards said.
Assisted dying is only available to patients that meet a range of eligibility criteria, including being over the age of 18, a resident for at least 12 months, and been diagnosed with a condition that is advanced, progressive and is expected to cause death within six months, or within 12 months in the case of neurodegenerative disease.
A patient must make three requests for assisted death, including once in writing, and have their eligibility assessed by two medical practitioners.
The minimum amount of time that the process can be completed, between a patient making the first request and actually completing voluntary assisted dying, is 9 days.
“Before it became legal we were getting (her application) ready to go,” Mr Edwards says.
“We had her mental assessment done, we came into hospital and got all that done, her mental capability (assessed). She signed a statutory declaration the other day on her mental capability. It has been a difficult process, but we were on to it early”.
Mr Edwards says his family did not find it overly difficult to access voluntary assisted dying in WA, however, he said some patients would struggle to complete the many steps involved without support.
“I understand why they’ve done it this way, but maybe a little bit more help would be nice,” he says.
Earlier this month, The WA Government has said it expected about 60 people to access voluntary assisted dying in the first 12 months of the program.
The state is the second to allow voluntary assisted dying after it became available in Victoria in 2019.
Parliaments in Tasmania and South Australia each passed voluntary assisted dying laws this year, but it won’t be available in those states for at least another year.
The Queensland Labor government introduced its voluntary assisted dying bill in May this year, while independent member for Sydney Alex Greenwich plans to introduce a bill for debate in the New South Wales parliament.
The Australian Capital Territory and the Northern Territory do not have the legislative power to pass laws about voluntary assisted dying.
"I am very happy"
Ms Passmore says she understands there will be some people across Australia that do not support her decision.
“I hope to God they will accept this as a valued part of our society,” she says.
“It’s a sad thing. Because I know there are many (people) that are suffering with pain, beyond pain. And they’re not allowed to make this decision”.
“There’s some naysayers everywhere, but I’m not waiting for naysayers. I’m fed up with the pain. I’m fed up with the suffering”.
Ms Passmore was in a de facto relationship at the time of her death and says not everyone in her family supported her decision.
But the steady stream of visitors kept coming to her hospital ward, until she died on Thursday morning.

During her final days, a photographic portrait of Ms Passmore from before the onset of MND hung on the wall in front of her hospital bed.
Ms Passmore looked at it, and thought about the life she had lived.
“I wont have to suffer anymore and this is the way I have chosen to die," she said.
"I am looking forward to the end. I am happy, very happy.”
Her family says she will be buried in Kalgoorlie, on Wongatha country alongside two brothers.
If you found this story upsetting please reach out to Beyond Blue on 1300 22 4636, Lifeline on 131114 or contact your local Aboriginal Medical Service.

